Key Words: Healthcare Disparities, Gender Role, Caregivers, Patients
Abstract
Introduction
In the Chilean health system, difficulties complicate womenÆs access to health care and aggravate the complexity of health-illness processes in their interaction as users or caregivers.
Objective
In the national and international literature, we aimed to identify gaps in womenÆs access to health care derived from gender disparities and the exercise of gender roles in a prioritized set of health problems. These problems exacerbate gender gaps and should be considered in health reform.
Methods
We made a literature review through algorithms, snowball sampling, and reference lists from November 2020 to March 2021. The population included were women of all ages, including women users of the health system and women caregivers of specific pathologies. The search was conducted in parallel by four investigators divided into two groups. It was cross-validated to ensure inter-investigator reliability by standardizing evidence eligibility criteria. The analysis showed women users' and caregivers' dimensions for a set of pathologies prioritized by the extent of the disease burden. The pathologies analyzed included stroke, obesity, depression, musculoskeletal pain, and breast cancer.
Results
Among women users of the health system, problems of access, rates of use, experience, and outcome for the whole group of prioritized pathologies were observed. In the women caregiver dimension, we found that women are the primary health care providers. There is a knowledge gap concerning obesity and musculoskeletal conditions. However, both were reported as health consequences of womenÆs caregiving roles.
Conclusion
The base problem, in both dimensions, is explained by biological, social, and cultural gender gaps that permeate the health care setting. Proposing a new health reform based only on the proposition of access to more benefits is insufficient according to the biopsychosocial context of women.
|
Main messages
|
Introduction
Issues concerning women and gender roles have gained importance in recent times and mainstreaming a gender perspective in different intersectoral policies. Gender is described as the socio-cultural environment of a person [1] attributing roles in different environments. For example, women are being poorly visible and valued in the health sector [2]. These socially ascribed roles have contributed to gender disparities.
The health sector organizes care by prioritizing health problems for access to health technologies and interventions (e.g., care, medicines, medical devices) [3]. These are covered through care regimens [4] that prioritize disease burden, cost-effectiveness, quality, safety, and effects on final health measures. Although these regimens introduce segmentation categories (children, adults, older adults, pregnant women, women of reproductive age), segmentation by gender role is not clearly seen. Thus, it is necessary to investigate whether women's experience due to gender differences and their gender role affect rates of service use, the experience of care, or health outcomes [5]. Despite the low economic exclusion of health insurance in Chile [6], women still have difficulties accessing care, which determines a complex health-illness process. Among Chilean women, the burden of disease is greater than men. The predominant causes of years of potential life lost are neuropsychiatric conditions (25.9%), and digestive (17.9%), cardiovascular (10.8%), and musculoskeletal diseases (6.5%) [7].
The overall objective of this report is to identify experience and care gaps related to gender disparities and the exercise of gender roles among women users and caregivers. This study is based on a targeted review of international and national (Chile) experience in a prioritized set of high magnitude health problems responsible for a high disease burden. This issue is addressed from community-based health care settings up to quaternary care. The secondary objective of the review is to explore the effects on utilization rates and health outcomes affected by such gender gaps.
The overall purpose of this literature review is to provide technical elements to support a local discussion in Chile on what gender differences should be recognized by the health system when prioritizing the sector's activity in future health reform.
Methods
A set of health problems were prioritized for which there is a sufficient body of evidence on their local characterization (according to magnitude - prevalence among the general population and women in the 2016/2017 and 2009/2010 Chilean National Health Survey), and disease burden (final health measures: years of life lost, disability-adjusted life years). The burden of disease data in Chile was compared and complemented with the Institute for Health Metrics and Evaluation databank report of the Institute for Health Metrics and Evaluation at the University of Washington [8] (Table 1).
Based on the triangulation of sources, we chose to address the following health problems: stroke, obesity, depression, musculoskeletal diseases, and breast cancer.
Table 1. Prioritization of relevant pathologies relating to womenÆs health and disease.
For the literature review, a search strategy was defined according to population (women of any age, women users of the health system, and women caregivers), concept (access gaps), and setting (from quaternary to community care in any country). Each pathology was analyzed from two dimensions:
- Women healthcare users exposed to gender disparities.
- Women caregivers tied to gender roles.
The possibility of adding emerging categories was left open.
A targeted search was conducted in PubMed/MEDLINE and Science Direct, plus web search engines (Google Scholar, Google). Additionally, the reference list of retrieved evidence was examined and supplemented with snowball sampling to improve scope and saturation.
We chose to add web search engines to control for publication bias of unpublished evidence. For example, in PubMed/MEDLINE, the combination of MeSH terms, free words, and Booleans was created to generate search algorithms such as the following:
(("gender role"[MeSH Terms]) OR ("gender"[All Fields] AND "role"[All Fields]) OR "gender role"[All Fields]) OR (("womans"[All Fields] OR "women"[MeSH Terms] OR "women"[All Fields] OR "woman"[All Fields] OR "women s"[All Fields] OR "womens"[All Fields]) AND ("role"[MeSH Terms] OR "role"[All Fields])) AND (("stroke"[MeSH Terms] OR "stroke"[All Fields] OR "strokes"[All Fields] OR "stroke s"[All Fields]) AND ("healthcare disparities"[MeSH Terms] OR ("healthcare"[All Fields] AND "disparities"[All Fields]) OR "healthcare disparities"[All Fields])) AND ((y_10[Filter]) AND (fft[Filter])).
The search was performed in parallel by four researchers in two groups and cross-validated for inter-investigator reliability between November 2020 and January 2021, mapping full-text articles in English and Spanish, up to ten years old, adjusted to the researcher's skills. This process was done to increase the body of evidence necessary to achieve the objectives of this study, especially in pathologies where gender research is scarce.
Results
After first- and second-level screening, 86 studies were mapped. Most are dated between 2001 and 2016 (n = 54, 62.8%) and come from the Americas (n = 51, 59.3%), with predominant quantitative designs (n = 35, 40.7%). The health problem with the highest number of referrals was stroke (n = 25), followed by obesity (n = 21) and breast cancer (n = 18). The healthcare user dimension contributed 58 studies, while the caregiver dimension contributed 28 (Table 2).
Table 2. Characterization of the evidence included in the literature review, according to dimension.
Healthcare user women exposed to gender disparities
Women users with a stroke
In Chile, stroke or cerebral thrombosis is on the rise in women, with an increase from 1.7% to 3.2%, although it is indicated that the difference is not significant [9].
Even though risk factors such as hypertension and smoking are more frequent in men, these increase the risk to a greater extent in women [10]. Women may be more predisposed to worse outcomes due to their previous burden of disease and sociodemographic factors [11]. Higher prevalences of hypertension are reported among affected women. These vary among studies with statistically significant differences ranging from 4.8 to 9.3% compared to men [12],[13],[14],[15],[16]. The same occurs with atrial fibrillation and diabetes [12],[15],[16],[17].
Stroke affects mostly men, but in women, its occurrence is more lethal and severe [18],[19]. In Australia, women suffered more severe strokes than men (44% versus 36%, P = 0.01) and with a higher 28-day mortality (31% versus 23%, P = 0.003) [20].
Stroke in women is associated with less specific symptoms [10], which may affect recognizing the disease and delay immediate transfer to health centers [10]. This phenomenon is associated with delayed diagnosis and fewer possible timely interventions [21] to restore cerebral blood flow (i.e., thrombolysis and mechanical thrombectomy). In the United States, women were less likely to be thrombolyzed than men (Odds ratio: 0.84; 95% confidence interval: 0.69 to 1.03) [22]. Only 66.3% of women received all the care for which they were eligible, compared with 71.1% of men (adjusted Odds ratio: 0.86; 95% confidence interval: 0.85 to 0.87) [23]. A European multicenter study also reported that the access to benefits was lower in women (P < 0.001), with disparities in access to brain imaging (77.1% in women versus 85.7% in men), Doppler (32.8% versus 44.0%), and angiography (5.5% versus 9.5%) [17].
In addition, greater complications and worse prognosis are observed in women survivors [18],[21],[24], with a higher frequency of depression, impaired quality of life, and care dependence [21]. Coma (P < 0.001), paralysis (P < 0.001), swallowing problems (P = 0.005), urinary incontinence (P < 0.001) and aphasia (P = 0.001) are more frequent in women [17]. The five-dimensional self-administered EuroQoL quality of life questionnaire, the EQ-5D (that assess mobility, self-care, activities of daily living, pain/discomfort, and anxiety/depression), found that in all of its categories, quality of life impairment was higher in women than in men (mean difference of -0.07 on a scale of 0 to 1) [25].
According to international data, women are 60% less likely to regain their independence and experience low access to rehabilitation (46%) [26] and have a greater disability (Odds ratio: 1.20, 95% confidence interval: 1.06 to 1.36) [25]. Women have a 3.5 times higher risk of hospitalizations given their level of disability. Stroke affects their role in the home, employment, community, interpersonal relationships, and independence [26].
Women users with obesity
In Chile, morbid obesity and obesity are higher in women than in men (4.7% versus 1.7%, and 33.7% versus 28.6%, respectively) [9] and is more frequent in people with less than eight years of schooling [9]. According to Atalah, low socioeconomic status in men is not associated with obesity in contrast to women [27]. In the United States, it was reported that women with access to low-quality diets were more likely to suffer from obesity or overweight (Odds ratio: 1.76; 95% confidence interval: 1.16 to 2.69) [28].
Obesity in Chilean women of childbearing age range from 20 to 35.3% [29],[30]. Pregnant women attending the Chilean public system show a sustained increasing trend over two decades, reaching an obesity prevalence of 31.4% in 2016 [31].
Many studies show the association of maternal obesity with adverse maternal and perinatal outcomes during gestation (e.g., weight alterations and preterm labor syndrome) and delivery (e.g., increased risk of cesarean section and delivery complications). This association with adverse outcomes is maintained long after pregnancy due to its transgenerational effect on the development of chronic diseases such as hypertension, diabetes, and metabolic syndrome [30],[32],[33],[34],[35],[36],[37].
In other countries, the aim has been to explore additional ways to solve obesity beyond prevention and nutrition. Not only has medication-based management gained strength, but access to surgical procedures is consolidating as a valid treatment alternative for obesity in its most severe state while being complemented by behavioral medicine-based management. Between 2013 and 2017, Chile reported a total of 9712 bariatric surgeries in collaborating centers, highlighting comorbidities such as hypertension (25%), diabetes (18%), musculoskeletal pain (8%), and depression (5%). At 12 months, sleeve gastrectomy decreased depression from 7 to 3.7%; hypertension from 41.7% to 22.3%; and musculoskeletal pain from 26.3% to 15.7% [38].
The bariatric surgery program of the National Health Fund, in almost a decade of implementation, provided access mainly to lower-income beneficiaries in bracket A (no income; 23.8%) and B (income less than or equal to 337 000 Chilean pesos, equivalent to US$ 496.8 at the exchange rate as of June 2021; 46.75%) [39]. In Chile, 85.4% of the bariatric surgeries in this program benefited women [39]. Similarly, 80.7% and 71.3% of these procedures are performed in women according to international and national studies, respectively [38],[40]. However, within the public sector, only slightly more than three thousand cases are known to have been funded by the public insurance program over eight years. These numbers correspond to 1.02 persons per day nationwide [39].
The role of surgical interventions in obesity is not cosmetic and less so in women. The maternal and perinatal prognosis after bariatric surgery is positive, although some evidence refutes this [41]. In a systematic review, pregnancy followed by surgery was associated with fewer complications. In diabetes, 0% of complications were reported compared to 22.1% of cohorts without the surgery (P < 0.05); and in preeclampsia, 0% of complications compared to 3.1% in those without the surgery (P < 0.05) [42]. The procedure may contribute to a decrease gestational and pregestational diabetes, hypertensive syndrome and preeclampsia; in addition to chronic hypertension complicating pregnancy [43], low birth weight (7.7% versus 10.6%; P < 0.05) and macrosomia (7.7% versus 14.6%; P < 0.05) [42].
It remains to demystify access to therapies that can reduce weight in women and reduce other pathologies with a high burden of disease in them and their offspring. It is worth exploring how coverage schemes and multidisciplinary teams accompany women with obesogenic habits, who have access to diets of low nutritional quality, live in poverty, or are in charge of single-parent households in their struggle to reduce weight.
Women users with depression
Mental health problems constitute the primary source of disease burden in Chile [44]. The incidence of depressive disorders is higher in women, presenting twice the risk of major depression [45]. About 30% of pregnant women suffer symptoms of depression and/or anxiety [44].
Grundy et al. analyzed depression among older adults (n = 2 649) in Santiago de Chile and found that the prevalence of depression was statistically higher in women than in men (36% versus 21%, P < 0.001) [46]. During 2019, the Ministry of Health evidenced a high prevalence of depressive symptoms in the population aged 65 years and older, with women presenting a higher prevalence of depressive symptomatology (16.9% versus 4.1% in men) [47].
In a Covid-19 social survey, 21.4% of people presented a moderate/severe level of anxiety and/or depression symptoms according to the Patient Health Questionnaire-4 (PHQ-4) scale. This percentage was higher in women than men (26% versus 16.5%) [48]. Depression in women is also mediated by hormonal factors, which increase the risk of depression during periods of hormonal transition (menarche, pregnancy, and menopause) [45],[49].
Women users with musculoskeletal diseases
According to the National Health Survey, 42.8% of women have a pain greater than or equal to 4 on a scale of 1 to 10, in contrast to 25.2% in men [50]. In women, pain in the knee (22%), lower back (16.3 to 22.1%), and shoulder (11.1%) [50],[51] are the most frequent.
The prevalence of pain is higher in women [52] and increases over 45 years of age (50.6%), being more frequent among low schooling women (46.6%) [50]. Likewise, chronic and/or persistent pain is more recurrent in women users [53], with one-third of them living with pain for periods of over five years [50]. A total of 83.3% of those affected who live with chronic pain perceive their health as "bad/very bad" [54].
Chronic pain impacts professional life. In Chile, 44.2% of women workers live with chronic pain [55]. While 60.7% of women have medical leave associated with chronic pain, in men, this percentage is reduced to 39.3 [51].
Long waiting times for diagnosis, less access to treatment or less effective treatment, greater use of antidepressants, and more frequent referrals to mental health professionals describe the gender bias existing in pain management among women compared to men [56]. Thus, feminist perspectives on managing chronic pain in women emerge, addressing polypharmacy and cultural norms in their treatment [57].
Women user with breast cancer
Breast cancer is recognized as the most commonly diagnosed cancer in women [58]. In Chile, its incidence is increasing. In 2018 alone, it was the leading cause of death in women, with 1511 deaths [59],[60].
In Chile, breast cancer is covered by the Explicit Health Guarantees regime for access to prioritized benefits for diagnosis, treatment (i.e., surgery, hormone therapy, chemotherapy, radiotherapy), and follow-up. A special fund creates a financial protection system for high-cost diagnoses and treatments (Ricarte Soto Law No. 20,850) for therapies aimed at a subgroup of patients, whose proportion is estimated to be less than 20% of the total number affected women [61]. There was no access to high-cost innovative treatments for women outside this subgroup that improve survival through the Explicit Health Guarantees or the Ricarte Soto Law. Affected women resort to courts of law to access prohibitively expensive drugs without coverage. A Chilean study reported that women perceive that the health system provides coverage for all breast cancer treatments through the Explicit Health Guarantees, lacking knowledge about gaps in coverage in deprioritized subgroups and specific molecular profiles [62]. It is expected that the new High-Cost Drugs Committee will address this problem.
Currently, new models are being sought to be adopted. For example, the "role of the navigator" proposes a professional accompaniment for informative actions, decision-making, and educational needs in women [63]. The information needs of the family circle are part of breast cancer care [64], having been documented in adolescent sons and daughters of women with breast cancer. In Chile, school support is emphasized as an extension of care outside the health sector [65] and the needs of professional help for sons, daughters, and partners of the diagnosed woman, promoting family-centered models of care [66].
Caregiver women tied to gender roles
Women caring for stroke survivors
In the United Kingdom and Brazil, the proportion of women caregiving stroke survivors ranges from 64.2% to 77% [67],[68],[69], and the majority of caregivers are males [68].
The burden of caregiving has been cited as moderate-severe in 65% of survivor caregivers [70], allocating 6.3 hours per day (95% confidence interval: 4.5 to 8.1 hours) to informal emotional, physical, and supervisory caregiving [68]. Also, the time spent is greater in women caregivers than in male caregivers (P = 0.002) [69]. The caregiver's health is lower than the general population [68]. Sleep disturbances, physical and psychological stress [70], and even depression and anxiety increase as the caregiving burden increases [71],[72].
The caregiving pressure decreases when the caregiver is male [68] and increases when the survivor's severity worsens. This burden is greater for wives [69]. Wives and daughters perceive a more significant caregiving burden than other relatives (P = 0.019) [70].
Women caregivers assume caregiving with baseline deficiencies in the knowledge that would enable them to provide care [73], especially at higher levels of dependency [70]. Thus, caregivers must self-educate themselves to exercise this role without proper support from the healthcare system.
Women caring for people with obesity
Morbid obesity challenges caregivers by increasing difficulty assisting with mobility, skincare, and hygiene of physically impaired individuals [74]. In the United States, 62.4% of older adult women had obesity compared to 37.6% of men (P < 0.001). Obese patients had less access to care for daily living activities [75].
Caregivers of obese and pre-bariatric patients had greater lower back, shoulder and wrist pain, which was more frequent in women caregivers [76]. In women caregivers of adolescent patients who benefited from bariatric surgery, limited family dysfunction is reported. In addition, bariatric surgery does not affect caregiver distress, parental stress, or family functioning [77].
Women caring for people with depression
In Canada (n = 23 404), the frequency of women caring for people with depression is higher than male caregivers (26 versus 16.2%; P < 0.001) [78]. Women caregivers have a greater illness, psychological distress, anxiety, and depression than in the control group, perceiving greater emotional and physical burden, with less social support [79].
Male caregivers report caring for people with physical health problems (71.9% versus 66%; P < 0.001), while women caregivers do so mostly in mental health problems (7.7% versus 6.4%; P < 0.001) [78].
Women caregivers may develop depression, and there is insufficient evidence on who provides care for women with depression [80]. However, depressive symptoms in older adults are associated with having a male caregiver (P = 0.006) [81].
Women caring for people with musculoskeletal pain
The evidence focuses mainly on the musculoskeletal consequences of caregiving. In Japan, it is described that 78.2% of women caregivers have experienced low back pain associated with nighttime caregiving activities, changes in the position of the cared-for family member, problematic behaviors, and medication intake [82]. More women (81.8%) are caregivers of children when they have a disability, being more prone to low back pain and disability while caring [83]. Women with low back pain do not stop fulfilling other social and family roles. Nor do they decrease their housework burden (P < 0.05) [84].
Older women workers have a high risk of experiencing low back pain. Some contributing factors are work-family imbalance, exposure to a hostile work environment, and job insecurity. The occupations where women were most at risk of developing pain were agriculture, fishing and, forestry [85].
Women caring for people with breast cancer
Breast cancer impacts the family dynamics since women often have multiple roles: partner, mother, primary source of income and/or caregiver. When the main caregiver requires care, it is another woman, and it is usually a daughter who assumes the task [86],[87],[88],[89],[90], which is not exempt from physical and psychological health damage [91]. The World Health Organization indicates that many women who become ill with breast cancer and caregivers postpone or do not carry out their treatments so their family budget is not compromised [92],[93].
In Mexico, the concept of reciprocity of care is proposed when the cared-for woman provides emotional care to the caregiver. Despite their disease, these women continue to exercise a caregiving role to family members [94].
Discussion
The problems of access faced by women are based on a set of social inequities. Although Chile has a very high human development index [95], it falls to 17.8% when adjusted for inequality. The gender development index for 2018, in terms of gross national income per capita, was $29 933 for men, in contrast to $15 211 for women [95]. According to the Organization for Economic Cooperation and Development, the wage gap in Chile between men and women is 46.4 versus 38.1% average in member states [96], added to gaps in access to work (38.2% in women versus 61.8% in men), and higher unemployment [97],[98].
Extreme and non-extreme poverty is higher among women than among men [99]. When the woman is head of household, extreme poverty increases to 9.2% versus 6.4% in households headed by a man [100]. According to the National Institute of Statistics, 25.4% of women in 1992 were heads of household, a figure that increased 2.8 times in 2017 [101]. Moreover, 55.7% of women-headed households are single-parent [102].
The role of the caregiving women is invisibilized, stereotyped, and usually unpaid [103],[104],[105]. Moreover, it is fulfilled in a context of multi-role and physical and emotional exhaustion [103],[106].
Women caregivers present almost twice as much overload as male caregivers [107]. In Chile, from the total number of caregivers (n = 4313), there are more women than men (66.8% vs 33.2%; P < 0.05), with an average age of 56.5 years (standard deviation: 16.14) [108]. According to the latest National Time Use Survey of the Chilean National Institute of Statistics, employed, unemployed, or inactive women spend at least twice as many hours per day (5.89 hours) on unpaid work compared to men (2.74 hours) [109].
How can the health system address the present gender gaps among women who are users of health services and/or caregivers?
Almost a decade ago, the Economic Commission for Latin America and the Caribbean recommended incorporating a gender perspective in health programs in Chile [110]. Income inequalities open up spaces to propose contributions to social security, which reduce women's expenditure. Meanwhile, they can establish exercises to identify and prioritize benefits to resolve gaps and even regulate differentiated co-payments given the present inequalities.
The 'Chile Crece Contigo' social protection subsystem is oriented to the comprehensive protection of children, with the mission of accompanying, protecting, and supporting boys, girls, and families. This is done through universal actions and services, focusing support on those who present greater vulnerability. The latter is a step forward in the multisectoral approach for the comprehensive protection of children from gestation onwards. This same approach should be extended to other pathologies beyond a woman's role as a mother. The women's health program of the Chilean Ministry of Health has been an effort to prioritize sexual and reproductive health problems. However, the mainstreaming of gender and gender role has not permeated other health problems. In the regime of Explicit Health Guarantees, the approach to health problems between men and women and the exercise of gender roles is mainly undifferentiated. In it, financing is articulated to cover benefits and is not necessarily intended to solve health gaps. The latter would imply considering medical benefits, but also activities to solve gender gaps.
Women have access to health services while simultaneously taking care of children or the sick. Health plans (and the sizing of the services offered by providers in agreements with health insurance companies) should consider a greater offer of services for women. At the same time, these plans and providers should face the non-medical costs of their care.
The approach to care in some programs of the National Service for the Prevention and Rehabilitation of Drug and Alcohol Use provides rehabilitation services to women as users. It supports gender role needs when they are mothers [111]. This approach recognizes non-medical costs that act as access barriers for women. A cost study of such a model indicated that outpatient treatments for women were more expensive than treatments for the general population. The research reported differences of up to 313 053 Chilean pesos, equivalent to US$462.5 per month per patient, at the 2016 annual period exchange rate. In these, spending on food for users and their children implied 6.31% of the indirect cost. To avoid discontinuation of treatment, the centers had to face the following costs: mobilization of users, feeding of children, cradles and baby-changing facilities, and an accompaniment to health check-ups of the son or daughter and the user, and court appearances. Rehabilitation not only involves financing health care (psychiatric consultations, psychodiagnosis, antidepressants), but also supporting the gender role of women [111].
Limitations
In this literature review, the research and availability of evidence using a gender perspective and focusing on gender gaps may bias the interpretation of results. It should be noted that this review reports on care gaps in women users of the health system and caregivers. However, men can also play a gender role that involves caregiving. The latter aspect makes it necessary to articulate responses of accompaniment in health-illness processes, regardless of the sex of the subject of rights.
In addition, although the fact that this review is based primarily on international references may also be a limitation, in the absence of more Chilean evidence, this approach serves as a trigger for discussion.
Conclusions
The evidence shows access gaps in women users and caregivers within pathologies of high disease burden. All this translates into different rates of care access, treatment, and health outcomes (e.g., disability, quality of life). The underlying problem seems to be explained by biological, social, and cultural gender gaps that permeate the health care environment.
Given the exercise of different gender roles, the health sector should recognize that it is necessary to consolidate comprehensive therapeutic models and approaches in social security, aiming at effective formulas for prioritization, health insurance, and gap resolution.
Women's health care has different needs, even more so when they exercise specific gender roles. It is necessary to discuss how Chile will allow a better approach to these gender gaps in view of the constitutional discussion and health reform.
Notes
Contributor roles
DP: conceptualization of the report, methodological development, use of reference management software, verification of the reproducibility of the review process, formal analysis of the evidence review, research process, metadata production, manuscript writing and final editing, supervision, and administration of the research project. RL: verification of the reproducibility of the review process, formal analysis of the evidence review, research process, metadata production, manuscript writing and final editing. BC - CR: development of the methodology, use of reference management software, verification of the reproducibility of the review process, formal analysis of the evidence review, research process, metadata production, manuscript writing, and final writing and editing.
Competing interests
Analysis carried out in alliance between Academics from Universidad de Chile, Academics from Universidad Andrés Bello, and Medtronic Chile. The authors have completed the ICMJE conflict of interest declaration form and declare that they have received support from Medtronic to fund the journal processing charges. The authors declare that they are fully responsible for the content of this article. Forms can be requested by contacting the responsible author or the Journal's editorial office.
Funding
Medtronic supported the present work by paying Medwave's processing charges.
Ethics
The present article is exempt from evaluation by an ethics committee because of the origin of the study design, which corresponds to a review of the literature (study in secondary sources of available literature).
Data sharing statement
Authors declare that they are willing to share data or any information of interest from the manuscript. Contact the corresponding author.
Language of submission
Spanish.
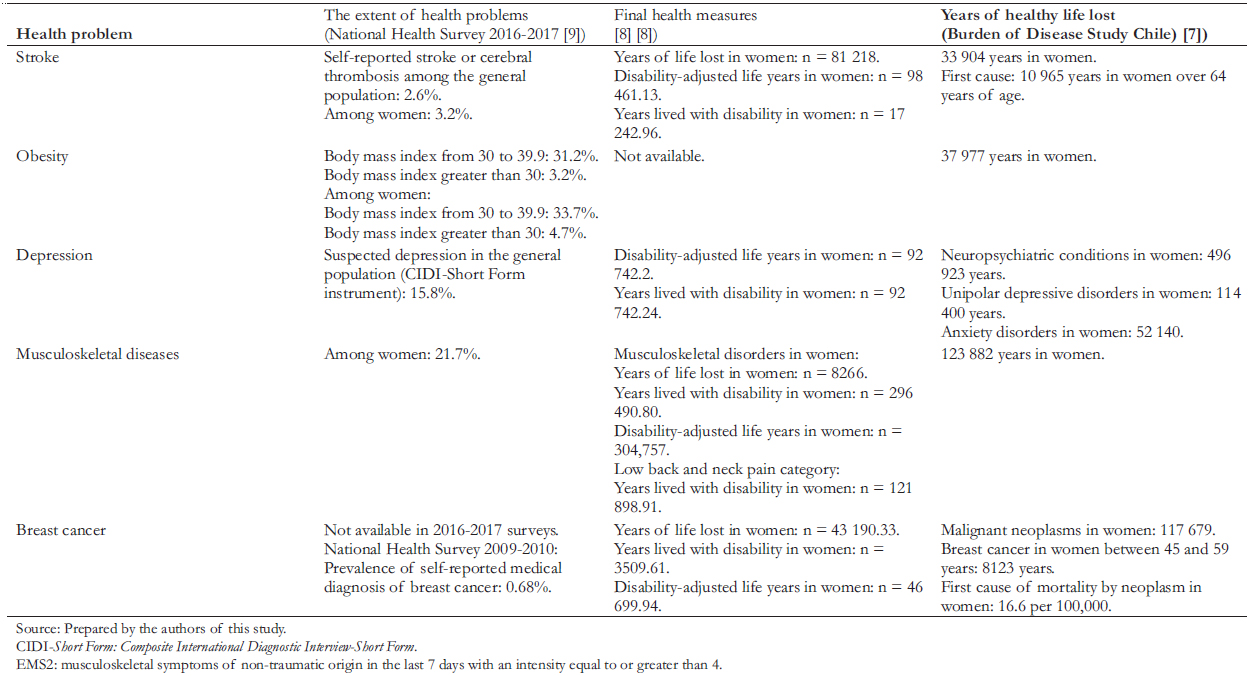
 Table 1. Prioritization of relevant pathologies relating to womenÆs health and disease.
Table 1. Prioritization of relevant pathologies relating to womenÆs health and disease.

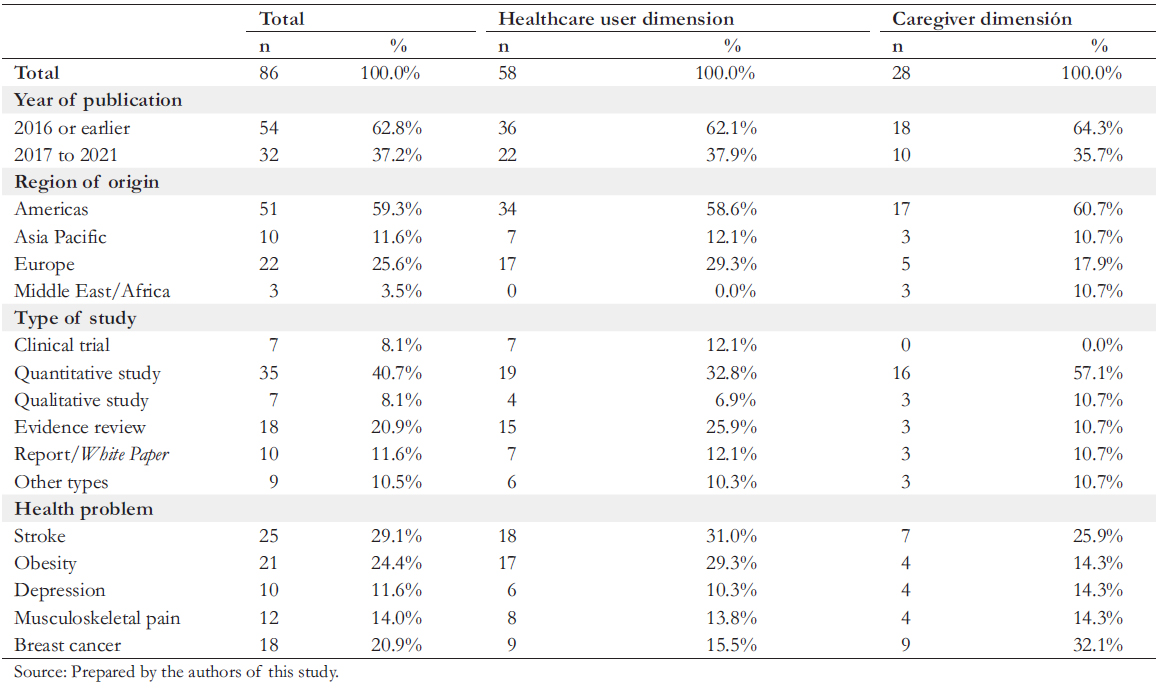 Table 2. Characterization of the evidence included in the literature review, according to dimension.
Table 2. Characterization of the evidence included in the literature review, according to dimension.

Introducci¾n
En el sistema de salud chileno persisten dificultades que complejizan el acceso de mujeres de forma efectiva a las atenciones de salud, o bien, derivan en que experimenten procesos de salud-enfermedad mßs complejos en su interacci¾n como usuarias o cuidadoras.
Objetivo
Identificamos en la literatura nacional e internacional, brechas de acceso a la atenci¾n de salud en la mujer derivadas de disparidades de gķnero y/o ejercicio del rol de gķnero, en un conjunto priorizado de problemas de salud. Estos problemas contribuyen a la problematizaci¾n de las brechas de gķnero a ser consideradas en la reforma de salud.
Mķtodos
Hicimos una revisi¾n de la literatura a travķs de algoritmos, muestreo en bola de nieve y listas de referencias, desde noviembre de 2020 hasta marzo de 2021. La poblaci¾n de anßlisis fueron mujeres de todas las edades usuarias de prestaciones de salud y cuidadoras en las mismas patologĒas abordadas. La b·squeda fue desarrollada en paralelo por cuatro investigadores, en dos grupos. Fue validada de forma cruzada asegurando la confiabilidad interevaluadores, estandarizando criterios de elegibilidad de la evidencia. El anßlisis se muestra en dimensiones de mujer usuaria y cuidadora, para un conjunto de patologĒas priorizadas por magnitud y carga de enfermedad: accidente vascular cerebral, obesidad, depresi¾n, dolor musculoesquelķtico y cßncer de mama.
Resultados
En la dimensi¾n de mujer usuaria, para todo el grupo de patologĒas priorizadas se observan problemas de acceso, tasas de uso, experiencia y resultados. Desde la dimensi¾n de mujer cuidadora, la mujer ejerce principalmente los cuidados de salud. Existe un vacĒo en la literatura en relaci¾n con la obesidad y afecciones musculoesquelķticas. Sin embargo, ambas se reportaron como consecuencias de salud en su rol de cuidadora.
Conclusi¾n
El problema en la base, en ambas dimensiones, queda explicado por brechas de gķnero biol¾gicas, sociales y culturales que permean el ßmbito de cuidados sanitarios. Proponer una nueva reforma de salud que solo se funde en la proposici¾n de acceso a mßs prestaciones, es insuficiente de acuerdo con el contexto biopsicosocial de la mujer.
 Authors:
Daniela Paredes-Fernßndez[1], Rony Lenz-Alcayaga[2], Camila Rojas-Cßceres[3], MarĒa Bego±a Carroza Escobar[4]
Authors:
Daniela Paredes-Fernßndez[1], Rony Lenz-Alcayaga[2], Camila Rojas-Cßceres[3], MarĒa Bego±a Carroza Escobar[4]
Affiliation:
[1] EconomĒa de la Salud y PolĒtica en Salud, Conglomerado PaĒses Latinoamķrica Sur, Medtronic, Santiago, Chile
[2] N·cleo Acadķmico Instituto de Salud P·blica, Universidad Andrķs Bello. Santiago, Chile
[3] Departamento de Promoci¾n de la Salud de la Mujer y el Reciķn Nacido, Facultad de Medicina, Universidad de Chile, Santiago, Chile
[4] Departamento de Promoci¾n de la Salud de la Mujer y el Reciķn Nacido, Facultad de Medicina, Universidad de Chile, Santiago, Chile
E-mail: daniela.m.paredes@medtronic.com

Citation: Paredes-Fernßndez D, Lenz-Alcayaga R, Rojas-Cßceres C, Carroza Escobar MB. WomenÆs access to health care: Gaps that the future health care reform in Chile must solve. Medwave 2021;21(10):e8490 doi: 10.5867/medwave.2021.10.8490
Submission date: 19/4/2021
Acceptance date: 14/9/2021
Publication date: 23/11/2021
Origin: Not commissioned
Type of review: Externally peer-reviewed by three reviewers, double-blind in the first round of review, and single-blind in the subsequent rounds

Comments (0)
We are pleased to have your comment on one of our articles. Your comment will be published as soon as it is posted. However, Medwave reserves the right to remove it later if the editors consider your comment to be: offensive in some sense, irrelevant, trivial, contains grammatical mistakes, contains political harangues, appears to be advertising, contains data from a particular person or suggests the need for changes in practice in terms of diagnostic, preventive or therapeutic interventions, if that evidence has not previously been published in a peer-reviewed journal.
No comments on this article.
To comment please log in
 Medwave provides HTML and PDF download counts as well as other harvested interaction metrics.
Medwave provides HTML and PDF download counts as well as other harvested interaction metrics. There may be a 48-hour delay for most recent metrics to be posted.

- Global Health 50/50. Gender equality: Flying blind in a time of crisis. 2021 Global Health 50/50 Report. Londres, Inglaterra; 2021. | Link |
- Guterres A. La disparidad de poder entre los gķneros. United Nations; 2020. | Link |
- Vergara-Iturriaga M, MartĒnez-Gutiķrrez MS. Financiamiento del sistema de salud chileno. Salud Publica Mex. 2006;48:512¢21. | CrossRef |
- Paredes-Fernßndez D, Lenz-Alcayaga R, Hernßndez-Sßnchez K, Quiroz-Carre±o J. Characterization and analysis of the basic elements of health payment mechanisms and their most frequent types. Medwave 2020;20(9):e8041 | CrossRef |
- Vega MJ, Bedregal GP, Jadue HL, DelgadoI. Gender inequity in the access to health care in Chile. Rev médica Chile. 2003;131: 669¢78. | CrossRef |
- Ministerio de Desarrollo Social de Chile. Encuesta CASEN: Salud. Razones de no atenci¾n mķdica ante enfermedad o accidente en los ·ltimos 3 meses. 2017. [on line] | Link |
- Ministerio de Salud de Chile. Estudio de carga de enfermedad y carga atribuible, Chile 2007. Santiago, Chile; 2008. | Link |
- Institute for Health Metrics and Evaluation (IHME). Chile: Country profile. What causes Most death Disabil. Comb. 2019. | Link |
- Gobierno de Chile, Ministerio de Salud. Encuesta Nacional de Salud 2016-2017. Primeros resultados. 2019. [on line] | Link |
- Girijala RL, Sohrabji F, Bush RL. Sex differences in stroke: Review of current knowledge and evidence. Vasc Med. 2017;22:135¢145. | CrossRef |
- Petrea RE, Beiser AS, Seshadri S, Kelly-Hayes M, Kase CS, Wolf PA, et al. Gender differences in stroke incidence and poststroke disability in the Framingham heart study. Stroke. 2009;40:1032¢7. | CrossRef |
- Anderson CS, Robinson T, Lindley RI, Arima H, Lavados PM, Lee T-H, et al. Low-Dose versus Standard-Dose Intravenous Alteplase in Acute Ischemic Stroke. N Engl J Med. 2016;374: 2313¢23. | CrossRef |
- Anderson CS, Huang Y, Wang JG, Arima H, Neal B, Peng B, et al. Intensive blood pressure reduction in acute cerebral haemorrhage trial (INTERACT): a randomised pilot trial. Lancet Neurol. 2008;7:91¢9. | CrossRef |
- Anderson CS, Heeley E, Huang Y, Wang J, Stapf C, Delcourt C, et al. Rapid Blood-Pressure Lowering in Patients with Acute Intracerebral Hemorrhage. N Engl J Med. 2013;368: 2355¢65. | CrossRef |
- Anderson CS, Arima H, Lavados P, Billot L, Hackett ML, OlavarrĒa VV, et al. Cluster-Randomized, Crossover Trial of Head Positioning in Acute Stroke. N Engl J Med. 2017;376: 2437¢2447. | CrossRef |
- Sandset EC, Bath PM, Boysen G, Jatuzis D, K§rv J, L³ders S, et al. The angiotensin-receptor blocker candesartan for treatment of acute stroke (SCAST): a randomised, placebo-controlled, double-blind trial. The Lancet. 2011;377: 741¢750. | CrossRef |
- Di Carlo A, Lamassa M, Baldereschi M, Pracucci G, Basile AM, Wolfe CDA, et al. Sex differences in the clinical presentation, resource use, and 3-month outcome of acute stroke in Europe: data from a multicenter multinational hospital-based registry. Stroke. 2003;34: 1114¢9. | CrossRef |
- Santalucia P, Pezzella FR, Sessa M, Monaco S, Torgano G, Anticoli S, et al. Sex differences in clinical presentation, severity and outcome of stroke: Results from a hospital-based registry. Eur J Intern Med. 2013;24: 167¢71. | CrossRef |
- Contreras JP, Pķrez O, Figueroa N. Cerebrovascular disease in women: state of the art and a cardiologistÆs perspective. Rev Colomb Cardiol 2018;25:113¢9. | CrossRef |
- Gall SL, Donnan G, Dewey HM, Macdonell R, Sturm J, Gilligan A, et al. Sex differences in presentation, severity, and management of stroke in a population-based study. Neurology. 2010;74: 975¢81. | CrossRef |
- Appelros P, Stegmayr B, Terķnt A. A review on sex differences in stroke treatment and outcome. Acta Neurol Scand. 2010;121: 359¢69. | CrossRef |
- Reed SD, Cramer SC, Blough DK, Meyer K, Jarvik JG. Treatment with tissue plasminogen activator and inpatient mortality rates for patients with ischemic stroke treated in community hospitals. Stroke. 2001;32: 1832¢40. | CrossRef |
- Reeves MJ, Fonarow GC, Zhao X, Smith EE, Schwamm LH, Get With The Guidelines-Stroke Steering Committee & Investigators. Quality of care in women with ischemic stroke in the GWTG program. Stroke. 2009;40: 1127¢33. | CrossRef |
- Persky RW, Turtzo LC, McCullough LD. Stroke in Women: Disparities and Outcomes. Curr Cardiol Rep. 2010;12: 6¢13. | CrossRef |
- Carcel C, Wang X, Sandset C, Delcourt C, Harima H, Lindley R, et al. Sex differences in treatment and outcome after stroke. Neurology. 2019;93. | CrossRef |
- Heart. Stroke Report: Lives disrupted: The impact of stroke on women. Canadß; 2018. | Link |
- Atalah E. Anßlisis de la situaci¾n nutricional de la poblaci¾n de Santiago. Rev médica Chile. 1993;121: 819¢26.
- Wolongevicz DM, Zhu L, Pencina MJ, Kimokoti RW, Newby PK, DÆAgostino RB, et al. Diet quality and obesity in women: the Framingham Nutrition Studies. Br J Nutr. 2010;103: 1223¢9. | CrossRef |
- Nozue M, Miyoshi M, Okumura J, Sanchez H, Handreu J, Chushi K. Prevalence and determinants of obesity and dietary habits among adults in rural area, Chile. Biosci Trends. 2007;3: 140¢8.
- Araya Bannout MA, Padilla O, Garmendia ML, Atalah E, Uauy R. Obesidad en mujeres Chilenas en edad fķrtil. Rev Med Chil. 2014;142: 1440¢8. | CrossRef |
- Gobierno de Chile. Vigilancia del estado nutricional de la poblaci¾n bajo control y de la lactancia materna en el Sistema P·blico de Salud de Chile. 2017. | Link |
- Papachatzi E, Paparrodopoulos S, Papadopoulos V, Dimitriou G, Vantarakis A. Pre-pregnancy maternal obesity in Greece: A case-control analysis. Early Hum Dev. 2016;93: 57¢61. | CrossRef |
- Zhou Y, Blustein J, Li H, Ye R, Zhu L, Liu J. Maternal Obesity, Caesarean Delivery and Caesarean Delivery on Maternal Request: A Cohort Analysis from China. Paediatr Perinat Epidemiol.2015;29: 232¢40. | CrossRef |
- Persson M, Pasupathy D, Hanson U, Westgren M, Norman M. Pre-pregnancy body mass index and the risk of adverse outcome in type 1 diabetic pregnancies: a population-based cohort study. BMJ Open. 2012;2. | CrossRef |
- He X-J, Dai R-X, Hu C-L. Maternal prepregnancy overweight and obesity and the risk of preeclampsia: A meta-analysis of cohort studies. Obes Res Clin Pract. 2020;14: 27¢33. | CrossRef |
- OÆReilly JR, Reynolds RM. The risk of maternal obesity to the long-term health of the offspring. Clin Endocrinol. 2013;78: 9¢16. | CrossRef |
- Carroza Escobar MB, Ortiz Contreras J, Bertoglia MP, Araya Bannout M. Pregestational obesity, maternal morbidity and risk of caesarean delivery in a country in an advanced stage of obstetric transition. Obesity Research & Clinical Practice. 2021;15: 73¢77. | CrossRef |
- International Federation for the Surgery of Obesity. The IFSO Global Registry. 2017.
- Paredes D, Lenz Alcayaga R, Quiroz Carre±o J, Hernandez K. Value Hel. 2020;23. | CrossRef |
- Young MT, Phelan MJ, Nguyen NT. A Decade Analysis of Trends and Outcomes of Male vs Female Patients Who Underwent Bariatric Surgery. J Am Coll Surg. 2016;222: 226¢31. | CrossRef |
- Akhter Z, Rankin J, Ceulemans D, Ngongalah L, Ackroyd R, Devlieger R, et al. Pregnancy after bariatric surgery and adverse perinatal outcomes: A systematic review and meta-analysis. PLOS Med. 2019;16. | CrossRef |
- Maggard MA, Yermilov I, Li Z, Maglione M, Newberry S, Suttorp M, et al. Pregnancy and fertility following bariatric surgery: a systematic review. JAMA. 2008;300: 2286¢96. | CrossRef |
- Ferrer-Mßrquez A. CirugĒa Barißtrica previo a embarazo y su impacto en el resultado perinatal. ARS MEDICA Rev Ciencias Mķdicas 2016;41:34¢41. | CrossRef |
- Gobierno de Chile, Ministerio de Salud. Plan nacional de salud mental 2017 - 2025. Santiago, Chile; 2017. | Link |
- Park LT, Zarate CA Jr. Depression in the Primary Care Setting. Reply. N Engl J Med. 2019;380: 2279¢2280. | CrossRef |
- Grundy EM, Albala C, Allen E, Dangour AD, Elbourne D, Uauy R. Grandparenting and psychosocial health among older Chileans: A longitudinal analysis. Aging Ment Health. 2012;16: 1047¢57. | CrossRef |
- Moreno-Gonzßlez MM, Galarza-Tejada DM, Tejada-Tayabas LM. Experiencias del cuidado familiar durante el cßncer de mama: la perspectiva de los cuidadores. Rev da Esc Enferm da USP 2019;53. | CrossRef |
- Ministerio de Salud de Chile. Actualizaci¾n Manual de GeriatrĒa para mķdicos. Santiago, Chile; 2019. | Link |
- Ministerio de Desarrollo Social y Familia de Chile. Resumen principales resultados. 2019. | Link |
- OÆBrien SM, Fitzgerald P, Scully P, Landers A, Scott LV, Dinan TG, et al. Impact of Gender and Menstrual Cycle Phase on Plasma Cytokine Concentrations. Neuroimmunomodulation. 2007;14: 84¢90. | CrossRef |
- Ministerio de Salud de Chile. Encuesta Nacional de Salud. Chile 2009-2010. Santiago; 2010. | CrossRef |
- Bilbeny N, Miranda JP, Eberhard ME, Ahumada M, Mķndez L, Orellana ME, et al. Survey of chronic pain in Chile - Prevalence and treatment, impact on mood, daily activities and quality of life. Scand J Pain. 2018;18: 449¢456. | CrossRef |
- Casals M, Samper D. EpidemiologĒa, prevalencia y calidad de vida del dolor cr¾nico no oncol¾gico. Rev la Soc Esp del Dolor. 2004;11: 260¢9.
- Kennedy J, Roll JM, Schraudner T, Murphy S, McPherson S, et al. Prevalence of persistent pain in the U.S. adult population: New data from the 2010 national health interview survey. J Pain. 2014;15: 979¢84. | CrossRef |
- Pereira LV, de Vasconcelos PP, Souza LAF, Pereira G de A, Nakatani AYK, Bachion MM. Prevalence and intensity of chronic pain and self-perceived health among elderly people: A population-based study. Rev Lat Am Enfermagem. 2014;22: 662¢9. | CrossRef |
- Bilbeny N. Dolor cr¾nico en Chile. Rev Mķdica ClĒnica Las Condes 2019;30:397¢406. | CrossRef |
- Samulowitz A, Gremyr I, Eriksson E, Hensing G. ōBrave Menö and ōEmotional Womenö: A Theory-Guided Literature Review on Gender Bias in Health Care and Gendered Norms towards Patients with Chronic Pain. Pain Res Manag. 2018;2018: 6358624. | CrossRef |
- Vearrier L. A Feminist Perspective on Gender Justice in the Treatment of Chronic Pain. Arch Med. 2016;8.
- World Health Organization. International Agency for Research on Cancer. Ginebra, Suiza; 2018. | Link |
- Ministerio de Salud de Chile. Plan Nacional de Cßncer 2018-2028. Santiago, Chile; 2018. | Link |
- Departamento de EstadĒstica e Informaci¾n de Salud (DEIS). EstadĒsticas de defunciones por causa bßsica de muerte; 2020. | Link |
- Del Castillo C, Cabrera ME, Derio PL. Resultados del tratamiento del cßncer de mama, Programa Nacional de Cßncer del Adulto. Rev Med Chile 2017;145:1507¢13. | CrossRef |
- Paredes D, Lenz R. Cßpsulas de comunicaci¾n cientĒfico-tķcnicas: mensajes claves para profesionales y pacientes. Una propuesta de divulgaci¾n para los casos de trastuzumab SC vs IV, ocrelizumab y pertuzumab en el sistema de salud chileno. Santiago, Chile; 2018.
- Till JE. Evaluation of support groups for women with breast cancer: importance of the navigator role. Health Qual Life Outcomes. 2003;1. | CrossRef |
- Forrest G, Plumb C, Ziebland S, Stein A. Breast cancer in the family--childrenÆs perceptions of their motherÆs cancer and its initial treatment: qualitative study. BMJ. 2006;332: 998¢1003. | CrossRef |
- Kristjanson LJ, Chalmers KI, Woodgate R. Information and support needs of adolescent children of women with breast cancer. Oncol Nurs Forum. 2004;31: 111¢9. | CrossRef |
- Forrest G, Plumb C, Ziebland S, Stein A. Breast cancer in young families: a qualitative interview study of fathers and their role and communication with their children following the diagnosis of maternal breast cancer. Psychooncology. 2009;18: 96¢103. | CrossRef |
- McCullagh E, Brigstocke G, Donaldson N, Kalra L. Determinants of caregiving burden and quality of life in caregivers of stroke patients. Stroke. 2005;36: 2181¢6. | CrossRef |
- Bugge C, Alexander H, Hagen S. Stroke patientsÆ informal caregivers. Patient, caregiver, and service factors that affect caregiver strain. Stroke. 1999;30: 1517¢23. | CrossRef |
- Carod-Artal FJ, Ferreira Coral L, Trizotto DS, Menezes Moreira C. Burden and perceived health status among caregivers of stroke patients. Cerebrovasc Dis. 2009;28: 472¢80. | CrossRef |
- Menon B, Salini P, Habeeba K, Conjeevaram J, Munisusmitha K. Female Caregivers and Stroke Severity Determines Caregiver Stress in Stroke Patients. Ann Indian Acad Neurol. 2017;20: 418¢424. | CrossRef |
- Denno MS, Gillard PJ, Graham GD, DiBonaventura MD, Goren A, Varon SF, et al. Anxiety and depression associated with caregiver burden in caregivers of stroke survivors with spasticity. Arch Phys Med Rehabil. 2013;94:1731¢6. | CrossRef |
- Saban KL, Mathews HL, Bryant FB, OÆBrien TE, Janusek LW. Depressive symptoms and diurnal salivary cortisol patterns among female caregivers of stroke survivors. Biol Res Nurs. 2012;14: 396¢404. | CrossRef |
- Saban KL, Hogan NS. Female caregivers of stroke survivors: coping and adapting to a life that once was. J Neurosci Nurs.2012;44: 2¢14. | CrossRef |
- Hahler B. Morbid obesity: a nursing care challenge. Dermatol Nurs. 2002;14: 255¢6.
- Ankuda CK, Harris J, Ornstein K, Levine DA, Langa KM, Kelley AS. Caregiving for Older Adults with Obesity in the United States. J Am Geriatr Soc. 2017;65: 1939¢1945. | CrossRef |
- Galinsky T, Deter L, Krieg E, Feng HA, Battaglia C, Bell R, et al. Safe patient handling and mobility (SPHM) for increasingly bariatric patient populations: Factors related to caregiversÆ self-reported pain and injury. Appl Ergon. 2021;91: 103300. | CrossRef |
- Zeller MH, Guilfoyle SM, Reiter-Purtill J, Ratcliff MB, Inge TH, Long JD. Adolescent bariatric surgery: caregiver and family functioning across the first postoperative year. Surg Obes Relat Dis. 2011;7: 145¢50. | CrossRef |
- Penning MJ, Wu Z. Caregiver Stress and Mental Health: Impact of Caregiving Relationship and Gender. Gerontologist. 2016;56: 1102¢1113. | CrossRef |
- Manso Martinez ME, Sanchez Lopez M, Cuellar Flores I. Salud y sobrecarga percibida en personas cuidadoras familiares de una zona rural. ClĒnica y Salud. 2013;24: 37¢45.
- EUFAMI. Encuesta cuidando de quienescuidan [c4c]: experiencias de cuidadores/as familiares de personas que vivencon trastorno mental grave: una investigaci¾n internacional. 2015. pp. 29¢31. | Link |
- Paskulin LMG, Bierhals CCBK, Santos NO dos. Depressive symptoms of the elderly people and caregiverÆs burden in home care. Investig y Educ en EnfermerĒa 2017;35:210¢20. | CrossRef |
- Suzuki K, Tamakoshi K, Sakakibara H. Caregiving activities closely associated with the development of low-back pain among female family caregivers. J Clin Nurs. 2016;25: 2156¢67. | CrossRef |
- Zamora MAL, Labao HC. Correlates of low back pain among Filipino caregivers of children with disability: A preliminary study. EnfermerĒa ClĒnica 020;30:120¢3. | CrossRef |
- Sheffer CE, Cassisi JE, Ferraresi LM, et al. Sex Differences in the Presentation of Chronic Low Back Pain. Psychol Women Q 2002;26:329¢40. | CrossRef |
- Departamento de Estudios de la Direcci¾n del Trabajo de Chile. Informe de Resultados Octava Encuesta Laboral: Inequidades y brechas de gķnero en el empleo. Encuesta laboral. 2014. | Link |
- Hernßndez L. La mujer con cßncer de mama: una experiencia desde la perspectiva del cuidado humano.EnfermerĒa Univ 2016;13:253¢9. | CrossRef |
- Carrasco C, BorderĒas C, Torns T. El trabajo de cuidados ┐responsabilidad compartida? 2011. | Link |
- Kusi G, Boamah Mensah AB, Boamah Mensah K, Dzomeku VM, Apiribu F, Duodu PA, et al. The experiences of family caregivers living with breast cancer patients in low-and middle-income countries: a systematic review. Syst Rev. 2020;9. | CrossRef |
- Kusi G, Boamah Mensah AB, Boamah Mensah K, Dzomeku VM, Apiribu F, Duodu PA. Caregiving motivations and experiences among family caregivers of patients living with advanced breast cancer in Ghana. PLoS One. 2020;15. | CrossRef |
- Vento F, Esposito MY, Vazquez R. CaracterĒsticas sociodemogrßficas de cuidadores primarios de mujeres con cßncer de mama y clĒnicas de las pacientes que atendĒan. Rev Cuba Enfermer 2015;31. | CrossRef |
- Ghaleb J, Al-Atuyyat N. Quality of life among primary caregivers of women with breast cancer: A review. Middle East J Cancer. 2013;4: 45¢459. | Link |
- Organizaci¾n Mundial de la Salud. Informe sobre los resultados de la OMS: presupuestos por programa 2016-2017. Ginebra, Suiza; 2018. | Link |
- Parra Giordano D, SaldĒas Fernßndez MA. Gesti¾n en Salud del Programa de Cßncer de Mama en Chile. EnfermerĒa actual en Costa Rica 2020;2118:1¢16. | CrossRef |
- Programa de las Naciones Unidas para el Desarrollo. Desigualdades del desarrollo humano en el siglo XXI: Chile. 2019. | Link |
- Organizaci¾n para la Cooperaci¾n y el Desarrollo Econ¾micos. La nueva Estrategia de empleo de la OCDE: Empleo de calidad para todos en un entorno laboral cambiante. Situaci¾n de Chile. 2018. | Link |
- Gobierno de Chile, Departamento de estudios de la Direcci¾n del trabajo. Informe de Resultados Octava Encuesta Laboral Inequidades y brechas de gķnero en el empleo. 2016. | Link |
- Instituto Nacional de EstadĒsticas. Gķnero y empleo. Santiago, Chile.: 2016. | Link |
- Gobierno de Chile, Ministerio de Desarrollo Social. Encuesta Casen 2015-2017. Trabajo Obs Soc. 2020. | Link |
- Gobierno de Chile, Ministerio de Desarrollo Social. Encuesta Casen 2015-2017. Pobreza Obs Soc. 2020. | Link |
- Gobierno de Chile, Instituto Nacional de Estadisticas. Hogares segun sexo del jefe de hogar Censos de 1992, 2002 y 2017; 2017. | Link |
- Gobierno de Chile, Ministerio de Desarrollo Social. 3a Encuesta Longitudinal de Primera Infancia ELPI 2017. UNICEF. | Link |
- Vaquiro RodrĒguez S, Stiepovich Bertoni J. CUIDADO INFORMAL,UN RETO ASUMIDO POR LA MUJER. Cienc y enfermerĒa. 2010;16. | CrossRef |
- Horton R. Offline: Gender and global healthŚan inexcusable global failure. The Lancet. 2019;393: 511. | CrossRef |
- Jimķnez Ruiz I, Moya Nicolßs M. La cuidadora familiar: sentimiento de obligaci¾n naturalizado de la mujer a la hora de cuidar. EnfermerĒa Glob 2017;17:420. | CrossRef |
- Jofrķ A. V, Mendoza P. S. Toma de Decisiones en Salud en Mujeres Cuidadoras Informales. Cienc y enfermerĒa 2005;11:37¢49. | CrossRef |
- Garcia-Calvente MM, Mateo-Rodriguez I, Moroto-Navarro G. El impacto de cuidar en la salud y la calidad de vida de las mujeres. Gac Sanit. 2004;18: 83¢92. | Link |
- Fernßndez MB, Herrera MS. El efecto del cuidado informal en la salud de los cuidadores familiares de personas mayores dependientes en Chile. Rev Med Chil 2020;148:30¢6. | CrossRef |
- Gobierno de Chile, Instituto Nacional de EstadĒstica. Encuesta Nacional del Uso de Tiempo (ENUT) 2015. 2015. | Link |
- German Agency for Technical Cooperation, CEPAL, Naciones Unidas. Equidad de gķnero en el sistema de salud chileno. 2002. | Link |
- Instituto de Administraci¾n de Salud, Lenz R, Mu±oz A, Arce R. Estudio evaluaci¾n de costos de planes de tratamiento de personas con consumo problemßtico de drogas y alcohol para el servicio nacional para la prevenci¾n y rehabilitaci¾n del consumo de drogas y alcohol. 2016. | Link |
 Global Health 50/50. Gender equality: Flying blind in a time of crisis. 2021 Global Health 50/50 Report. Londres, Inglaterra; 2021. | Link |
Global Health 50/50. Gender equality: Flying blind in a time of crisis. 2021 Global Health 50/50 Report. Londres, Inglaterra; 2021. | Link | Vergara-Iturriaga M, MartĒnez-Gutiķrrez MS. Financiamiento del sistema de salud chileno. Salud Publica Mex. 2006;48:512¢21. | CrossRef |
Vergara-Iturriaga M, MartĒnez-Gutiķrrez MS. Financiamiento del sistema de salud chileno. Salud Publica Mex. 2006;48:512¢21. | CrossRef | Paredes-Fernßndez D, Lenz-Alcayaga R, Hernßndez-Sßnchez K, Quiroz-Carre±o J. Characterization and analysis of the basic elements of health payment mechanisms and their most frequent types. Medwave 2020;20(9):e8041 | CrossRef |
Paredes-Fernßndez D, Lenz-Alcayaga R, Hernßndez-Sßnchez K, Quiroz-Carre±o J. Characterization and analysis of the basic elements of health payment mechanisms and their most frequent types. Medwave 2020;20(9):e8041 | CrossRef | Vega MJ, Bedregal GP, Jadue HL, DelgadoI. Gender inequity in the access to health care in Chile. Rev médica Chile. 2003;131: 669¢78. | CrossRef |
Vega MJ, Bedregal GP, Jadue HL, DelgadoI. Gender inequity in the access to health care in Chile. Rev médica Chile. 2003;131: 669¢78. | CrossRef | Ministerio de Desarrollo Social de Chile. Encuesta CASEN: Salud. Razones de no atenci¾n mķdica ante enfermedad o accidente en los ·ltimos 3 meses. 2017. [on line] | Link |
Ministerio de Desarrollo Social de Chile. Encuesta CASEN: Salud. Razones de no atenci¾n mķdica ante enfermedad o accidente en los ·ltimos 3 meses. 2017. [on line] | Link | Ministerio de Salud de Chile. Estudio de carga de enfermedad y carga atribuible, Chile 2007. Santiago, Chile; 2008. | Link |
Ministerio de Salud de Chile. Estudio de carga de enfermedad y carga atribuible, Chile 2007. Santiago, Chile; 2008. | Link | Institute for Health Metrics and Evaluation (IHME). Chile: Country profile. What causes Most death Disabil. Comb. 2019. | Link |
Institute for Health Metrics and Evaluation (IHME). Chile: Country profile. What causes Most death Disabil. Comb. 2019. | Link | Gobierno de Chile, Ministerio de Salud. Encuesta Nacional de Salud 2016-2017. Primeros resultados. 2019. [on line] | Link |
Gobierno de Chile, Ministerio de Salud. Encuesta Nacional de Salud 2016-2017. Primeros resultados. 2019. [on line] | Link | Girijala RL, Sohrabji F, Bush RL. Sex differences in stroke: Review of current knowledge and evidence. Vasc Med. 2017;22:135¢145. | CrossRef |
Girijala RL, Sohrabji F, Bush RL. Sex differences in stroke: Review of current knowledge and evidence. Vasc Med. 2017;22:135¢145. | CrossRef | Petrea RE, Beiser AS, Seshadri S, Kelly-Hayes M, Kase CS, Wolf PA, et al. Gender differences in stroke incidence and poststroke disability in the Framingham heart study. Stroke. 2009;40:1032¢7. | CrossRef |
Petrea RE, Beiser AS, Seshadri S, Kelly-Hayes M, Kase CS, Wolf PA, et al. Gender differences in stroke incidence and poststroke disability in the Framingham heart study. Stroke. 2009;40:1032¢7. | CrossRef | Anderson CS, Robinson T, Lindley RI, Arima H, Lavados PM, Lee T-H, et al. Low-Dose versus Standard-Dose Intravenous Alteplase in Acute Ischemic Stroke. N Engl J Med. 2016;374: 2313¢23. | CrossRef |
Anderson CS, Robinson T, Lindley RI, Arima H, Lavados PM, Lee T-H, et al. Low-Dose versus Standard-Dose Intravenous Alteplase in Acute Ischemic Stroke. N Engl J Med. 2016;374: 2313¢23. | CrossRef | Anderson CS, Huang Y, Wang JG, Arima H, Neal B, Peng B, et al. Intensive blood pressure reduction in acute cerebral haemorrhage trial (INTERACT): a randomised pilot trial. Lancet Neurol. 2008;7:91¢9. | CrossRef |
Anderson CS, Huang Y, Wang JG, Arima H, Neal B, Peng B, et al. Intensive blood pressure reduction in acute cerebral haemorrhage trial (INTERACT): a randomised pilot trial. Lancet Neurol. 2008;7:91¢9. | CrossRef | Anderson CS, Heeley E, Huang Y, Wang J, Stapf C, Delcourt C, et al. Rapid Blood-Pressure Lowering in Patients with Acute Intracerebral Hemorrhage. N Engl J Med. 2013;368: 2355¢65. | CrossRef |
Anderson CS, Heeley E, Huang Y, Wang J, Stapf C, Delcourt C, et al. Rapid Blood-Pressure Lowering in Patients with Acute Intracerebral Hemorrhage. N Engl J Med. 2013;368: 2355¢65. | CrossRef | Anderson CS, Arima H, Lavados P, Billot L, Hackett ML, OlavarrĒa VV, et al. Cluster-Randomized, Crossover Trial of Head Positioning in Acute Stroke. N Engl J Med. 2017;376: 2437¢2447. | CrossRef |
Anderson CS, Arima H, Lavados P, Billot L, Hackett ML, OlavarrĒa VV, et al. Cluster-Randomized, Crossover Trial of Head Positioning in Acute Stroke. N Engl J Med. 2017;376: 2437¢2447. | CrossRef | Sandset EC, Bath PM, Boysen G, Jatuzis D, K§rv J, L³ders S, et al. The angiotensin-receptor blocker candesartan for treatment of acute stroke (SCAST): a randomised, placebo-controlled, double-blind trial. The Lancet. 2011;377: 741¢750. | CrossRef |
Sandset EC, Bath PM, Boysen G, Jatuzis D, K§rv J, L³ders S, et al. The angiotensin-receptor blocker candesartan for treatment of acute stroke (SCAST): a randomised, placebo-controlled, double-blind trial. The Lancet. 2011;377: 741¢750. | CrossRef | Di Carlo A, Lamassa M, Baldereschi M, Pracucci G, Basile AM, Wolfe CDA, et al. Sex differences in the clinical presentation, resource use, and 3-month outcome of acute stroke in Europe: data from a multicenter multinational hospital-based registry. Stroke. 2003;34: 1114¢9. | CrossRef |
Di Carlo A, Lamassa M, Baldereschi M, Pracucci G, Basile AM, Wolfe CDA, et al. Sex differences in the clinical presentation, resource use, and 3-month outcome of acute stroke in Europe: data from a multicenter multinational hospital-based registry. Stroke. 2003;34: 1114¢9. | CrossRef | Santalucia P, Pezzella FR, Sessa M, Monaco S, Torgano G, Anticoli S, et al. Sex differences in clinical presentation, severity and outcome of stroke: Results from a hospital-based registry. Eur J Intern Med. 2013;24: 167¢71. | CrossRef |
Santalucia P, Pezzella FR, Sessa M, Monaco S, Torgano G, Anticoli S, et al. Sex differences in clinical presentation, severity and outcome of stroke: Results from a hospital-based registry. Eur J Intern Med. 2013;24: 167¢71. | CrossRef | Contreras JP, Pķrez O, Figueroa N. Cerebrovascular disease in women: state of the art and a cardiologistÆs perspective. Rev Colomb Cardiol 2018;25:113¢9. | CrossRef |
Contreras JP, Pķrez O, Figueroa N. Cerebrovascular disease in women: state of the art and a cardiologistÆs perspective. Rev Colomb Cardiol 2018;25:113¢9. | CrossRef | Gall SL, Donnan G, Dewey HM, Macdonell R, Sturm J, Gilligan A, et al. Sex differences in presentation, severity, and management of stroke in a population-based study. Neurology. 2010;74: 975¢81. | CrossRef |
Gall SL, Donnan G, Dewey HM, Macdonell R, Sturm J, Gilligan A, et al. Sex differences in presentation, severity, and management of stroke in a population-based study. Neurology. 2010;74: 975¢81. | CrossRef | Appelros P, Stegmayr B, Terķnt A. A review on sex differences in stroke treatment and outcome. Acta Neurol Scand. 2010;121: 359¢69. | CrossRef |
Appelros P, Stegmayr B, Terķnt A. A review on sex differences in stroke treatment and outcome. Acta Neurol Scand. 2010;121: 359¢69. | CrossRef | Reed SD, Cramer SC, Blough DK, Meyer K, Jarvik JG. Treatment with tissue plasminogen activator and inpatient mortality rates for patients with ischemic stroke treated in community hospitals. Stroke. 2001;32: 1832¢40. | CrossRef |
Reed SD, Cramer SC, Blough DK, Meyer K, Jarvik JG. Treatment with tissue plasminogen activator and inpatient mortality rates for patients with ischemic stroke treated in community hospitals. Stroke. 2001;32: 1832¢40. | CrossRef | Reeves MJ, Fonarow GC, Zhao X, Smith EE, Schwamm LH, Get With The Guidelines-Stroke Steering Committee & Investigators. Quality of care in women with ischemic stroke in the GWTG program. Stroke. 2009;40: 1127¢33. | CrossRef |
Reeves MJ, Fonarow GC, Zhao X, Smith EE, Schwamm LH, Get With The Guidelines-Stroke Steering Committee & Investigators. Quality of care in women with ischemic stroke in the GWTG program. Stroke. 2009;40: 1127¢33. | CrossRef | Persky RW, Turtzo LC, McCullough LD. Stroke in Women: Disparities and Outcomes. Curr Cardiol Rep. 2010;12: 6¢13. | CrossRef |
Persky RW, Turtzo LC, McCullough LD. Stroke in Women: Disparities and Outcomes. Curr Cardiol Rep. 2010;12: 6¢13. | CrossRef | Carcel C, Wang X, Sandset C, Delcourt C, Harima H, Lindley R, et al. Sex differences in treatment and outcome after stroke. Neurology. 2019;93. | CrossRef |
Carcel C, Wang X, Sandset C, Delcourt C, Harima H, Lindley R, et al. Sex differences in treatment and outcome after stroke. Neurology. 2019;93. | CrossRef | Atalah E. Anßlisis de la situaci¾n nutricional de la poblaci¾n de Santiago. Rev médica Chile. 1993;121: 819¢26.
Atalah E. Anßlisis de la situaci¾n nutricional de la poblaci¾n de Santiago. Rev médica Chile. 1993;121: 819¢26.  Wolongevicz DM, Zhu L, Pencina MJ, Kimokoti RW, Newby PK, DÆAgostino RB, et al. Diet quality and obesity in women: the Framingham Nutrition Studies. Br J Nutr. 2010;103: 1223¢9. | CrossRef |
Wolongevicz DM, Zhu L, Pencina MJ, Kimokoti RW, Newby PK, DÆAgostino RB, et al. Diet quality and obesity in women: the Framingham Nutrition Studies. Br J Nutr. 2010;103: 1223¢9. | CrossRef | Nozue M, Miyoshi M, Okumura J, Sanchez H, Handreu J, Chushi K. Prevalence and determinants of obesity and dietary habits among adults in rural area, Chile. Biosci Trends. 2007;3: 140¢8.
Nozue M, Miyoshi M, Okumura J, Sanchez H, Handreu J, Chushi K. Prevalence and determinants of obesity and dietary habits among adults in rural area, Chile. Biosci Trends. 2007;3: 140¢8.  Araya Bannout MA, Padilla O, Garmendia ML, Atalah E, Uauy R. Obesidad en mujeres Chilenas en edad fķrtil. Rev Med Chil. 2014;142: 1440¢8. | CrossRef |
Araya Bannout MA, Padilla O, Garmendia ML, Atalah E, Uauy R. Obesidad en mujeres Chilenas en edad fķrtil. Rev Med Chil. 2014;142: 1440¢8. | CrossRef | Gobierno de Chile. Vigilancia del estado nutricional de la poblaci¾n bajo control y de la lactancia materna en el Sistema P·blico de Salud de Chile. 2017. | Link |
Gobierno de Chile. Vigilancia del estado nutricional de la poblaci¾n bajo control y de la lactancia materna en el Sistema P·blico de Salud de Chile. 2017. | Link | Papachatzi E, Paparrodopoulos S, Papadopoulos V, Dimitriou G, Vantarakis A. Pre-pregnancy maternal obesity in Greece: A case-control analysis. Early Hum Dev. 2016;93: 57¢61. | CrossRef |
Papachatzi E, Paparrodopoulos S, Papadopoulos V, Dimitriou G, Vantarakis A. Pre-pregnancy maternal obesity in Greece: A case-control analysis. Early Hum Dev. 2016;93: 57¢61. | CrossRef | Zhou Y, Blustein J, Li H, Ye R, Zhu L, Liu J. Maternal Obesity, Caesarean Delivery and Caesarean Delivery on Maternal Request: A Cohort Analysis from China. Paediatr Perinat Epidemiol.2015;29: 232¢40. | CrossRef |
Zhou Y, Blustein J, Li H, Ye R, Zhu L, Liu J. Maternal Obesity, Caesarean Delivery and Caesarean Delivery on Maternal Request: A Cohort Analysis from China. Paediatr Perinat Epidemiol.2015;29: 232¢40. | CrossRef | Persson M, Pasupathy D, Hanson U, Westgren M, Norman M. Pre-pregnancy body mass index and the risk of adverse outcome in type 1 diabetic pregnancies: a population-based cohort study. BMJ Open. 2012;2. | CrossRef |
Persson M, Pasupathy D, Hanson U, Westgren M, Norman M. Pre-pregnancy body mass index and the risk of adverse outcome in type 1 diabetic pregnancies: a population-based cohort study. BMJ Open. 2012;2. | CrossRef | He X-J, Dai R-X, Hu C-L. Maternal prepregnancy overweight and obesity and the risk of preeclampsia: A meta-analysis of cohort studies. Obes Res Clin Pract. 2020;14: 27¢33. | CrossRef |
He X-J, Dai R-X, Hu C-L. Maternal prepregnancy overweight and obesity and the risk of preeclampsia: A meta-analysis of cohort studies. Obes Res Clin Pract. 2020;14: 27¢33. | CrossRef | OÆReilly JR, Reynolds RM. The risk of maternal obesity to the long-term health of the offspring. Clin Endocrinol. 2013;78: 9¢16. | CrossRef |
OÆReilly JR, Reynolds RM. The risk of maternal obesity to the long-term health of the offspring. Clin Endocrinol. 2013;78: 9¢16. | CrossRef | Carroza Escobar MB, Ortiz Contreras J, Bertoglia MP, Araya Bannout M. Pregestational obesity, maternal morbidity and risk of caesarean delivery in a country in an advanced stage of obstetric transition. Obesity Research & Clinical Practice. 2021;15: 73¢77. | CrossRef |
Carroza Escobar MB, Ortiz Contreras J, Bertoglia MP, Araya Bannout M. Pregestational obesity, maternal morbidity and risk of caesarean delivery in a country in an advanced stage of obstetric transition. Obesity Research & Clinical Practice. 2021;15: 73¢77. | CrossRef | International Federation for the Surgery of Obesity. The IFSO Global Registry. 2017.
International Federation for the Surgery of Obesity. The IFSO Global Registry. 2017.  Young MT, Phelan MJ, Nguyen NT. A Decade Analysis of Trends and Outcomes of Male vs Female Patients Who Underwent Bariatric Surgery. J Am Coll Surg. 2016;222: 226¢31. | CrossRef |
Young MT, Phelan MJ, Nguyen NT. A Decade Analysis of Trends and Outcomes of Male vs Female Patients Who Underwent Bariatric Surgery. J Am Coll Surg. 2016;222: 226¢31. | CrossRef | Akhter Z, Rankin J, Ceulemans D, Ngongalah L, Ackroyd R, Devlieger R, et al. Pregnancy after bariatric surgery and adverse perinatal outcomes: A systematic review and meta-analysis. PLOS Med. 2019;16. | CrossRef |
Akhter Z, Rankin J, Ceulemans D, Ngongalah L, Ackroyd R, Devlieger R, et al. Pregnancy after bariatric surgery and adverse perinatal outcomes: A systematic review and meta-analysis. PLOS Med. 2019;16. | CrossRef | Maggard MA, Yermilov I, Li Z, Maglione M, Newberry S, Suttorp M, et al. Pregnancy and fertility following bariatric surgery: a systematic review. JAMA. 2008;300: 2286¢96. | CrossRef |
Maggard MA, Yermilov I, Li Z, Maglione M, Newberry S, Suttorp M, et al. Pregnancy and fertility following bariatric surgery: a systematic review. JAMA. 2008;300: 2286¢96. | CrossRef | Ferrer-Mßrquez A. CirugĒa Barißtrica previo a embarazo y su impacto en el resultado perinatal. ARS MEDICA Rev Ciencias Mķdicas 2016;41:34¢41. | CrossRef |
Ferrer-Mßrquez A. CirugĒa Barißtrica previo a embarazo y su impacto en el resultado perinatal. ARS MEDICA Rev Ciencias Mķdicas 2016;41:34¢41. | CrossRef | Gobierno de Chile, Ministerio de Salud. Plan nacional de salud mental 2017 - 2025. Santiago, Chile; 2017. | Link |
Gobierno de Chile, Ministerio de Salud. Plan nacional de salud mental 2017 - 2025. Santiago, Chile; 2017. | Link | Park LT, Zarate CA Jr. Depression in the Primary Care Setting. Reply. N Engl J Med. 2019;380: 2279¢2280. | CrossRef |
Park LT, Zarate CA Jr. Depression in the Primary Care Setting. Reply. N Engl J Med. 2019;380: 2279¢2280. | CrossRef | Grundy EM, Albala C, Allen E, Dangour AD, Elbourne D, Uauy R. Grandparenting and psychosocial health among older Chileans: A longitudinal analysis. Aging Ment Health. 2012;16: 1047¢57. | CrossRef |
Grundy EM, Albala C, Allen E, Dangour AD, Elbourne D, Uauy R. Grandparenting and psychosocial health among older Chileans: A longitudinal analysis. Aging Ment Health. 2012;16: 1047¢57. | CrossRef | Moreno-Gonzßlez MM, Galarza-Tejada DM, Tejada-Tayabas LM. Experiencias del cuidado familiar durante el cßncer de mama: la perspectiva de los cuidadores. Rev da Esc Enferm da USP 2019;53. | CrossRef |
Moreno-Gonzßlez MM, Galarza-Tejada DM, Tejada-Tayabas LM. Experiencias del cuidado familiar durante el cßncer de mama: la perspectiva de los cuidadores. Rev da Esc Enferm da USP 2019;53. | CrossRef | Ministerio de Salud de Chile. Actualizaci¾n Manual de GeriatrĒa para mķdicos. Santiago, Chile; 2019. | Link |
Ministerio de Salud de Chile. Actualizaci¾n Manual de GeriatrĒa para mķdicos. Santiago, Chile; 2019. | Link | OÆBrien SM, Fitzgerald P, Scully P, Landers A, Scott LV, Dinan TG, et al. Impact of Gender and Menstrual Cycle Phase on Plasma Cytokine Concentrations. Neuroimmunomodulation. 2007;14: 84¢90. | CrossRef |
OÆBrien SM, Fitzgerald P, Scully P, Landers A, Scott LV, Dinan TG, et al. Impact of Gender and Menstrual Cycle Phase on Plasma Cytokine Concentrations. Neuroimmunomodulation. 2007;14: 84¢90. | CrossRef | Ministerio de Salud de Chile. Encuesta Nacional de Salud. Chile 2009-2010. Santiago; 2010. | CrossRef |
Ministerio de Salud de Chile. Encuesta Nacional de Salud. Chile 2009-2010. Santiago; 2010. | CrossRef | Bilbeny N, Miranda JP, Eberhard ME, Ahumada M, Mķndez L, Orellana ME, et al. Survey of chronic pain in Chile - Prevalence and treatment, impact on mood, daily activities and quality of life. Scand J Pain. 2018;18: 449¢456. | CrossRef |
Bilbeny N, Miranda JP, Eberhard ME, Ahumada M, Mķndez L, Orellana ME, et al. Survey of chronic pain in Chile - Prevalence and treatment, impact on mood, daily activities and quality of life. Scand J Pain. 2018;18: 449¢456. | CrossRef | Casals M, Samper D. EpidemiologĒa, prevalencia y calidad de vida del dolor cr¾nico no oncol¾gico. Rev la Soc Esp del Dolor. 2004;11: 260¢9.
Casals M, Samper D. EpidemiologĒa, prevalencia y calidad de vida del dolor cr¾nico no oncol¾gico. Rev la Soc Esp del Dolor. 2004;11: 260¢9.  Kennedy J, Roll JM, Schraudner T, Murphy S, McPherson S, et al. Prevalence of persistent pain in the U.S. adult population: New data from the 2010 national health interview survey. J Pain. 2014;15: 979¢84. | CrossRef |
Kennedy J, Roll JM, Schraudner T, Murphy S, McPherson S, et al. Prevalence of persistent pain in the U.S. adult population: New data from the 2010 national health interview survey. J Pain. 2014;15: 979¢84. | CrossRef | Pereira LV, de Vasconcelos PP, Souza LAF, Pereira G de A, Nakatani AYK, Bachion MM. Prevalence and intensity of chronic pain and self-perceived health among elderly people: A population-based study. Rev Lat Am Enfermagem. 2014;22: 662¢9. | CrossRef |
Pereira LV, de Vasconcelos PP, Souza LAF, Pereira G de A, Nakatani AYK, Bachion MM. Prevalence and intensity of chronic pain and self-perceived health among elderly people: A population-based study. Rev Lat Am Enfermagem. 2014;22: 662¢9. | CrossRef | Samulowitz A, Gremyr I, Eriksson E, Hensing G. ōBrave Menö and ōEmotional Womenö: A Theory-Guided Literature Review on Gender Bias in Health Care and Gendered Norms towards Patients with Chronic Pain. Pain Res Manag. 2018;2018: 6358624. | CrossRef |
Samulowitz A, Gremyr I, Eriksson E, Hensing G. ōBrave Menö and ōEmotional Womenö: A Theory-Guided Literature Review on Gender Bias in Health Care and Gendered Norms towards Patients with Chronic Pain. Pain Res Manag. 2018;2018: 6358624. | CrossRef | Vearrier L. A Feminist Perspective on Gender Justice in the Treatment of Chronic Pain. Arch Med. 2016;8.
Vearrier L. A Feminist Perspective on Gender Justice in the Treatment of Chronic Pain. Arch Med. 2016;8.  World Health Organization. International Agency for Research on Cancer. Ginebra, Suiza; 2018. | Link |
World Health Organization. International Agency for Research on Cancer. Ginebra, Suiza; 2018. | Link | Departamento de EstadĒstica e Informaci¾n de Salud (DEIS). EstadĒsticas de defunciones por causa bßsica de muerte; 2020. | Link |
Departamento de EstadĒstica e Informaci¾n de Salud (DEIS). EstadĒsticas de defunciones por causa bßsica de muerte; 2020. | Link | Del Castillo C, Cabrera ME, Derio PL. Resultados del tratamiento del cßncer de mama, Programa Nacional de Cßncer del Adulto. Rev Med Chile 2017;145:1507¢13. | CrossRef |
Del Castillo C, Cabrera ME, Derio PL. Resultados del tratamiento del cßncer de mama, Programa Nacional de Cßncer del Adulto. Rev Med Chile 2017;145:1507¢13. | CrossRef | Paredes D, Lenz R. Cßpsulas de comunicaci¾n cientĒfico-tķcnicas: mensajes claves para profesionales y pacientes. Una propuesta de divulgaci¾n para los casos de trastuzumab SC vs IV, ocrelizumab y pertuzumab en el sistema de salud chileno. Santiago, Chile; 2018.
Paredes D, Lenz R. Cßpsulas de comunicaci¾n cientĒfico-tķcnicas: mensajes claves para profesionales y pacientes. Una propuesta de divulgaci¾n para los casos de trastuzumab SC vs IV, ocrelizumab y pertuzumab en el sistema de salud chileno. Santiago, Chile; 2018.  Till JE. Evaluation of support groups for women with breast cancer: importance of the navigator role. Health Qual Life Outcomes. 2003;1. | CrossRef |
Till JE. Evaluation of support groups for women with breast cancer: importance of the navigator role. Health Qual Life Outcomes. 2003;1. | CrossRef | Forrest G, Plumb C, Ziebland S, Stein A. Breast cancer in the family--childrenÆs perceptions of their motherÆs cancer and its initial treatment: qualitative study. BMJ. 2006;332: 998¢1003. | CrossRef |
Forrest G, Plumb C, Ziebland S, Stein A. Breast cancer in the family--childrenÆs perceptions of their motherÆs cancer and its initial treatment: qualitative study. BMJ. 2006;332: 998¢1003. | CrossRef | Kristjanson LJ, Chalmers KI, Woodgate R. Information and support needs of adolescent children of women with breast cancer. Oncol Nurs Forum. 2004;31: 111¢9. | CrossRef |
Kristjanson LJ, Chalmers KI, Woodgate R. Information and support needs of adolescent children of women with breast cancer. Oncol Nurs Forum. 2004;31: 111¢9. | CrossRef | Forrest G, Plumb C, Ziebland S, Stein A. Breast cancer in young families: a qualitative interview study of fathers and their role and communication with their children following the diagnosis of maternal breast cancer. Psychooncology. 2009;18: 96¢103. | CrossRef |
Forrest G, Plumb C, Ziebland S, Stein A. Breast cancer in young families: a qualitative interview study of fathers and their role and communication with their children following the diagnosis of maternal breast cancer. Psychooncology. 2009;18: 96¢103. | CrossRef | McCullagh E, Brigstocke G, Donaldson N, Kalra L. Determinants of caregiving burden and quality of life in caregivers of stroke patients. Stroke. 2005;36: 2181¢6. | CrossRef |
McCullagh E, Brigstocke G, Donaldson N, Kalra L. Determinants of caregiving burden and quality of life in caregivers of stroke patients. Stroke. 2005;36: 2181¢6. | CrossRef | Bugge C, Alexander H, Hagen S. Stroke patientsÆ informal caregivers. Patient, caregiver, and service factors that affect caregiver strain. Stroke. 1999;30: 1517¢23. | CrossRef |
Bugge C, Alexander H, Hagen S. Stroke patientsÆ informal caregivers. Patient, caregiver, and service factors that affect caregiver strain. Stroke. 1999;30: 1517¢23. | CrossRef | Carod-Artal FJ, Ferreira Coral L, Trizotto DS, Menezes Moreira C. Burden and perceived health status among caregivers of stroke patients. Cerebrovasc Dis. 2009;28: 472¢80. | CrossRef |
Carod-Artal FJ, Ferreira Coral L, Trizotto DS, Menezes Moreira C. Burden and perceived health status among caregivers of stroke patients. Cerebrovasc Dis. 2009;28: 472¢80. | CrossRef | Menon B, Salini P, Habeeba K, Conjeevaram J, Munisusmitha K. Female Caregivers and Stroke Severity Determines Caregiver Stress in Stroke Patients. Ann Indian Acad Neurol. 2017;20: 418¢424. | CrossRef |
Menon B, Salini P, Habeeba K, Conjeevaram J, Munisusmitha K. Female Caregivers and Stroke Severity Determines Caregiver Stress in Stroke Patients. Ann Indian Acad Neurol. 2017;20: 418¢424. | CrossRef | Denno MS, Gillard PJ, Graham GD, DiBonaventura MD, Goren A, Varon SF, et al. Anxiety and depression associated with caregiver burden in caregivers of stroke survivors with spasticity. Arch Phys Med Rehabil. 2013;94:1731¢6. | CrossRef |
Denno MS, Gillard PJ, Graham GD, DiBonaventura MD, Goren A, Varon SF, et al. Anxiety and depression associated with caregiver burden in caregivers of stroke survivors with spasticity. Arch Phys Med Rehabil. 2013;94:1731¢6. | CrossRef | Saban KL, Mathews HL, Bryant FB, OÆBrien TE, Janusek LW. Depressive symptoms and diurnal salivary cortisol patterns among female caregivers of stroke survivors. Biol Res Nurs. 2012;14: 396¢404. | CrossRef |
Saban KL, Mathews HL, Bryant FB, OÆBrien TE, Janusek LW. Depressive symptoms and diurnal salivary cortisol patterns among female caregivers of stroke survivors. Biol Res Nurs. 2012;14: 396¢404. | CrossRef | Saban KL, Hogan NS. Female caregivers of stroke survivors: coping and adapting to a life that once was. J Neurosci Nurs.2012;44: 2¢14. | CrossRef |
Saban KL, Hogan NS. Female caregivers of stroke survivors: coping and adapting to a life that once was. J Neurosci Nurs.2012;44: 2¢14. | CrossRef | Hahler B. Morbid obesity: a nursing care challenge. Dermatol Nurs. 2002;14: 255¢6.
Hahler B. Morbid obesity: a nursing care challenge. Dermatol Nurs. 2002;14: 255¢6.  Ankuda CK, Harris J, Ornstein K, Levine DA, Langa KM, Kelley AS. Caregiving for Older Adults with Obesity in the United States. J Am Geriatr Soc. 2017;65: 1939¢1945. | CrossRef |
Ankuda CK, Harris J, Ornstein K, Levine DA, Langa KM, Kelley AS. Caregiving for Older Adults with Obesity in the United States. J Am Geriatr Soc. 2017;65: 1939¢1945. | CrossRef | Galinsky T, Deter L, Krieg E, Feng HA, Battaglia C, Bell R, et al. Safe patient handling and mobility (SPHM) for increasingly bariatric patient populations: Factors related to caregiversÆ self-reported pain and injury. Appl Ergon. 2021;91: 103300. | CrossRef |
Galinsky T, Deter L, Krieg E, Feng HA, Battaglia C, Bell R, et al. Safe patient handling and mobility (SPHM) for increasingly bariatric patient populations: Factors related to caregiversÆ self-reported pain and injury. Appl Ergon. 2021;91: 103300. | CrossRef | Zeller MH, Guilfoyle SM, Reiter-Purtill J, Ratcliff MB, Inge TH, Long JD. Adolescent bariatric surgery: caregiver and family functioning across the first postoperative year. Surg Obes Relat Dis. 2011;7: 145¢50. | CrossRef |
Zeller MH, Guilfoyle SM, Reiter-Purtill J, Ratcliff MB, Inge TH, Long JD. Adolescent bariatric surgery: caregiver and family functioning across the first postoperative year. Surg Obes Relat Dis. 2011;7: 145¢50. | CrossRef | Penning MJ, Wu Z. Caregiver Stress and Mental Health: Impact of Caregiving Relationship and Gender. Gerontologist. 2016;56: 1102¢1113. | CrossRef |
Penning MJ, Wu Z. Caregiver Stress and Mental Health: Impact of Caregiving Relationship and Gender. Gerontologist. 2016;56: 1102¢1113. | CrossRef | Manso Martinez ME, Sanchez Lopez M, Cuellar Flores I. Salud y sobrecarga percibida en personas cuidadoras familiares de una zona rural. ClĒnica y Salud. 2013;24: 37¢45.
Manso Martinez ME, Sanchez Lopez M, Cuellar Flores I. Salud y sobrecarga percibida en personas cuidadoras familiares de una zona rural. ClĒnica y Salud. 2013;24: 37¢45.  EUFAMI. Encuesta cuidando de quienescuidan [c4c]: experiencias de cuidadores/as familiares de personas que vivencon trastorno mental grave: una investigaci¾n internacional. 2015. pp. 29¢31. | Link |
EUFAMI. Encuesta cuidando de quienescuidan [c4c]: experiencias de cuidadores/as familiares de personas que vivencon trastorno mental grave: una investigaci¾n internacional. 2015. pp. 29¢31. | Link | Paskulin LMG, Bierhals CCBK, Santos NO dos. Depressive symptoms of the elderly people and caregiverÆs burden in home care. Investig y Educ en EnfermerĒa 2017;35:210¢20. | CrossRef |
Paskulin LMG, Bierhals CCBK, Santos NO dos. Depressive symptoms of the elderly people and caregiverÆs burden in home care. Investig y Educ en EnfermerĒa 2017;35:210¢20. | CrossRef | Suzuki K, Tamakoshi K, Sakakibara H. Caregiving activities closely associated with the development of low-back pain among female family caregivers. J Clin Nurs. 2016;25: 2156¢67. | CrossRef |
Suzuki K, Tamakoshi K, Sakakibara H. Caregiving activities closely associated with the development of low-back pain among female family caregivers. J Clin Nurs. 2016;25: 2156¢67. | CrossRef | Zamora MAL, Labao HC. Correlates of low back pain among Filipino caregivers of children with disability: A preliminary study. EnfermerĒa ClĒnica 020;30:120¢3. | CrossRef |
Zamora MAL, Labao HC. Correlates of low back pain among Filipino caregivers of children with disability: A preliminary study. EnfermerĒa ClĒnica 020;30:120¢3. | CrossRef | Sheffer CE, Cassisi JE, Ferraresi LM, et al. Sex Differences in the Presentation of Chronic Low Back Pain. Psychol Women Q 2002;26:329¢40. | CrossRef |
Sheffer CE, Cassisi JE, Ferraresi LM, et al. Sex Differences in the Presentation of Chronic Low Back Pain. Psychol Women Q 2002;26:329¢40. | CrossRef | Departamento de Estudios de la Direcci¾n del Trabajo de Chile. Informe de Resultados Octava Encuesta Laboral: Inequidades y brechas de gķnero en el empleo. Encuesta laboral. 2014. | Link |
Departamento de Estudios de la Direcci¾n del Trabajo de Chile. Informe de Resultados Octava Encuesta Laboral: Inequidades y brechas de gķnero en el empleo. Encuesta laboral. 2014. | Link | Hernßndez L. La mujer con cßncer de mama: una experiencia desde la perspectiva del cuidado humano.EnfermerĒa Univ 2016;13:253¢9. | CrossRef |
Hernßndez L. La mujer con cßncer de mama: una experiencia desde la perspectiva del cuidado humano.EnfermerĒa Univ 2016;13:253¢9. | CrossRef | Carrasco C, BorderĒas C, Torns T. El trabajo de cuidados ┐responsabilidad compartida? 2011. | Link |
Carrasco C, BorderĒas C, Torns T. El trabajo de cuidados ┐responsabilidad compartida? 2011. | Link | Kusi G, Boamah Mensah AB, Boamah Mensah K, Dzomeku VM, Apiribu F, Duodu PA, et al. The experiences of family caregivers living with breast cancer patients in low-and middle-income countries: a systematic review. Syst Rev. 2020;9. | CrossRef |
Kusi G, Boamah Mensah AB, Boamah Mensah K, Dzomeku VM, Apiribu F, Duodu PA, et al. The experiences of family caregivers living with breast cancer patients in low-and middle-income countries: a systematic review. Syst Rev. 2020;9. | CrossRef | Kusi G, Boamah Mensah AB, Boamah Mensah K, Dzomeku VM, Apiribu F, Duodu PA. Caregiving motivations and experiences among family caregivers of patients living with advanced breast cancer in Ghana. PLoS One. 2020;15. | CrossRef |
Kusi G, Boamah Mensah AB, Boamah Mensah K, Dzomeku VM, Apiribu F, Duodu PA. Caregiving motivations and experiences among family caregivers of patients living with advanced breast cancer in Ghana. PLoS One. 2020;15. | CrossRef | Vento F, Esposito MY, Vazquez R. CaracterĒsticas sociodemogrßficas de cuidadores primarios de mujeres con cßncer de mama y clĒnicas de las pacientes que atendĒan. Rev Cuba Enfermer 2015;31. | CrossRef |
Vento F, Esposito MY, Vazquez R. CaracterĒsticas sociodemogrßficas de cuidadores primarios de mujeres con cßncer de mama y clĒnicas de las pacientes que atendĒan. Rev Cuba Enfermer 2015;31. | CrossRef | Ghaleb J, Al-Atuyyat N. Quality of life among primary caregivers of women with breast cancer: A review. Middle East J Cancer. 2013;4: 45¢459. | Link |
Ghaleb J, Al-Atuyyat N. Quality of life among primary caregivers of women with breast cancer: A review. Middle East J Cancer. 2013;4: 45¢459. | Link | Organizaci¾n Mundial de la Salud. Informe sobre los resultados de la OMS: presupuestos por programa 2016-2017. Ginebra, Suiza; 2018. | Link |
Organizaci¾n Mundial de la Salud. Informe sobre los resultados de la OMS: presupuestos por programa 2016-2017. Ginebra, Suiza; 2018. | Link | Parra Giordano D, SaldĒas Fernßndez MA. Gesti¾n en Salud del Programa de Cßncer de Mama en Chile. EnfermerĒa actual en Costa Rica 2020;2118:1¢16. | CrossRef |
Parra Giordano D, SaldĒas Fernßndez MA. Gesti¾n en Salud del Programa de Cßncer de Mama en Chile. EnfermerĒa actual en Costa Rica 2020;2118:1¢16. | CrossRef | Programa de las Naciones Unidas para el Desarrollo. Desigualdades del desarrollo humano en el siglo XXI: Chile. 2019. | Link |
Programa de las Naciones Unidas para el Desarrollo. Desigualdades del desarrollo humano en el siglo XXI: Chile. 2019. | Link | Organizaci¾n para la Cooperaci¾n y el Desarrollo Econ¾micos. La nueva Estrategia de empleo de la OCDE: Empleo de calidad para todos en un entorno laboral cambiante. Situaci¾n de Chile. 2018. | Link |
Organizaci¾n para la Cooperaci¾n y el Desarrollo Econ¾micos. La nueva Estrategia de empleo de la OCDE: Empleo de calidad para todos en un entorno laboral cambiante. Situaci¾n de Chile. 2018. | Link | Gobierno de Chile, Departamento de estudios de la Direcci¾n del trabajo. Informe de Resultados Octava Encuesta Laboral Inequidades y brechas de gķnero en el empleo. 2016. | Link |
Gobierno de Chile, Departamento de estudios de la Direcci¾n del trabajo. Informe de Resultados Octava Encuesta Laboral Inequidades y brechas de gķnero en el empleo. 2016. | Link | Gobierno de Chile, Ministerio de Desarrollo Social. Encuesta Casen 2015-2017. Trabajo Obs Soc. 2020. | Link |
Gobierno de Chile, Ministerio de Desarrollo Social. Encuesta Casen 2015-2017. Trabajo Obs Soc. 2020. | Link | Gobierno de Chile, Ministerio de Desarrollo Social. Encuesta Casen 2015-2017. Pobreza Obs Soc. 2020. | Link |
Gobierno de Chile, Ministerio de Desarrollo Social. Encuesta Casen 2015-2017. Pobreza Obs Soc. 2020. | Link | Gobierno de Chile, Instituto Nacional de Estadisticas. Hogares segun sexo del jefe de hogar Censos de 1992, 2002 y 2017; 2017. | Link |
Gobierno de Chile, Instituto Nacional de Estadisticas. Hogares segun sexo del jefe de hogar Censos de 1992, 2002 y 2017; 2017. | Link | Gobierno de Chile, Ministerio de Desarrollo Social. 3a Encuesta Longitudinal de Primera Infancia ELPI 2017. UNICEF. | Link |
Gobierno de Chile, Ministerio de Desarrollo Social. 3a Encuesta Longitudinal de Primera Infancia ELPI 2017. UNICEF. | Link | Vaquiro RodrĒguez S, Stiepovich Bertoni J. CUIDADO INFORMAL,UN RETO ASUMIDO POR LA MUJER. Cienc y enfermerĒa. 2010;16. | CrossRef |
Vaquiro RodrĒguez S, Stiepovich Bertoni J. CUIDADO INFORMAL,UN RETO ASUMIDO POR LA MUJER. Cienc y enfermerĒa. 2010;16. | CrossRef | Horton R. Offline: Gender and global healthŚan inexcusable global failure. The Lancet. 2019;393: 511. | CrossRef |
Horton R. Offline: Gender and global healthŚan inexcusable global failure. The Lancet. 2019;393: 511. | CrossRef | Jimķnez Ruiz I, Moya Nicolßs M. La cuidadora familiar: sentimiento de obligaci¾n naturalizado de la mujer a la hora de cuidar. EnfermerĒa Glob 2017;17:420. | CrossRef |
Jimķnez Ruiz I, Moya Nicolßs M. La cuidadora familiar: sentimiento de obligaci¾n naturalizado de la mujer a la hora de cuidar. EnfermerĒa Glob 2017;17:420. | CrossRef | Jofrķ A. V, Mendoza P. S. Toma de Decisiones en Salud en Mujeres Cuidadoras Informales. Cienc y enfermerĒa 2005;11:37¢49. | CrossRef |
Jofrķ A. V, Mendoza P. S. Toma de Decisiones en Salud en Mujeres Cuidadoras Informales. Cienc y enfermerĒa 2005;11:37¢49. | CrossRef | Garcia-Calvente MM, Mateo-Rodriguez I, Moroto-Navarro G. El impacto de cuidar en la salud y la calidad de vida de las mujeres. Gac Sanit. 2004;18: 83¢92. | Link |
Garcia-Calvente MM, Mateo-Rodriguez I, Moroto-Navarro G. El impacto de cuidar en la salud y la calidad de vida de las mujeres. Gac Sanit. 2004;18: 83¢92. | Link | Fernßndez MB, Herrera MS. El efecto del cuidado informal en la salud de los cuidadores familiares de personas mayores dependientes en Chile. Rev Med Chil 2020;148:30¢6. | CrossRef |
Fernßndez MB, Herrera MS. El efecto del cuidado informal en la salud de los cuidadores familiares de personas mayores dependientes en Chile. Rev Med Chil 2020;148:30¢6. | CrossRef | Gobierno de Chile, Instituto Nacional de EstadĒstica. Encuesta Nacional del Uso de Tiempo (ENUT) 2015. 2015. | Link |
Gobierno de Chile, Instituto Nacional de EstadĒstica. Encuesta Nacional del Uso de Tiempo (ENUT) 2015. 2015. | Link | German Agency for Technical Cooperation, CEPAL, Naciones Unidas. Equidad de gķnero en el sistema de salud chileno. 2002. | Link |
German Agency for Technical Cooperation, CEPAL, Naciones Unidas. Equidad de gķnero en el sistema de salud chileno. 2002. | Link | Instituto de Administraci¾n de Salud, Lenz R, Mu±oz A, Arce R. Estudio evaluaci¾n de costos de planes de tratamiento de personas con consumo problemßtico de drogas y alcohol para el servicio nacional para la prevenci¾n y rehabilitaci¾n del consumo de drogas y alcohol. 2016. | Link |
Instituto de Administraci¾n de Salud, Lenz R, Mu±oz A, Arce R. Estudio evaluaci¾n de costos de planes de tratamiento de personas con consumo problemßtico de drogas y alcohol para el servicio nacional para la prevenci¾n y rehabilitaci¾n del consumo de drogas y alcohol. 2016. | Link |Systematization of initiatives in sexual and reproductive health about good practices criteria in response to the COVID-19 pandemic in primary health care in Chile
Clinical, psychological, social, and family characterization of suicidal behavior in Chilean adolescents: a multiple correspondence analysis









